Life with a C-Spine Injury: How to Avoid Respiratory Complications
A cervical spine injury can change your life in an instant. These injuries, sometimes called C-spine injuries, are the most severe form of spinal cord injuries, affecting the widest range of bodily functions. Though most C-spine injury survivors experience similar symptoms, spinal cord injuries are unpredictable. Some people spontaneously recover from their injuries; others make little progress even with quality physical therapy and dedicated medical care.
Reasonable expectations, coupled with a clear understanding of spinal cord anatomy, can help to prepare you for the recovery journey while equipping you to be a strong advocate for yourself.
What Is a Cervical Spinal Cord Injury?
A cervical spinal cord injury is the term for any kind of injury that impacts the C1-C7 sections of the cervical spine—i.e. the vertebrae in the neck.
There are many kinds of injuries that can lead to a cervical SCI, such as complete and incomplete cervical spinal cord injuries, ligament C-spine injuries, spinal lesions, and more. The sheer variety of SCI types can make it nearly impossible to create an accurate prognosis for a cervical spinal cord injury. So, it’s important to not give up too early because of a premature prognosis—especially one coming from a non-expert!
Understanding Spinal Cord Anatomy
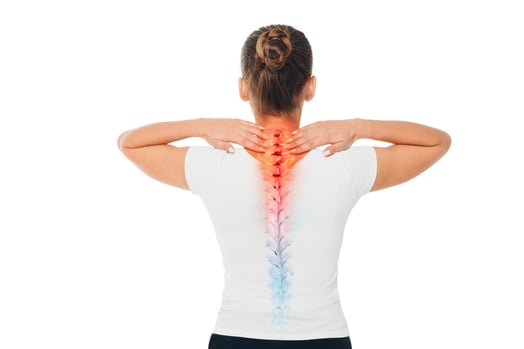 The spinal cord is the body's relay center, sending messages from the brain to various parts of the body, and consolidating signals to send back to the brain. It also coordinates reflexes, so damage to the spinal cord can significantly impede function—even if the rest of the body is healthy.
The spinal cord is the body's relay center, sending messages from the brain to various parts of the body, and consolidating signals to send back to the brain. It also coordinates reflexes, so damage to the spinal cord can significantly impede function—even if the rest of the body is healthy.
The spinal cord is protected by 24 vertebrae, numbered 1-24 in descending order. Most doctors divide the spinal cord into four distinct regions, again in descending order: the cervical spine, thoracic spine, and the lumbar spine. The lowest region of the spinal column is known as the sacrum, which doesn’t technically contain the spinal cord proper, but it does contain some spinal nerve bundles.
In short, an injury to vertebra C-4 would be significantly higher on the spine (and is likely to be more limiting) than a similar injury to the T-3 or L-5 spinal cord vertebrae.
Causes of Cervical Spinal Cord Injuries
There are many potential causes for a cervical SCI. Data from the National Spinal Cord Injury Statistical Center (NSCISC) highlights following as the leading causes of spinal cord injuries:
- Vehicular crashes (38.6%)
- Falls (32.2%)
- Acts of violence (14%)
- Sports-related injuries (7.8%)
- Medical/surgical procedures (4.2%)
- Other assorted causes (3.2%)
While the NSCISC’s data is for all spinal cord injury causes, it is still useful for describing the common causes of cervical spinal cord injuries.
Whiplash injuries of the cervical spine are frequently caused by car accidents. This is because the head may move rapidly during a crash, stressing or breaking the vertebrae of the neck as the skull whips back-and-forth or side-to-side.
As for sports injuries, why wouldn’t you remove the helmet of an injured player with a suspected cervical spine injury? Simply because the motions caused could exacerbate the SCI—potentially turning an incomplete SCI or simple cracked vertebrae into a complete (and potentially fatal) injury.
Cervical Spine Injuries and Paralysis
Injuries to the cervical spinal cord typically produce the most extensive disabilities. This region of the spinal cord plays a key role in the body’s most vital functions, including breathing, and controls most motor skills below the site of the injury. Thus, a cervical spinal cord injury frequently causes paralysis below the site of the injury, including of the arms and legs.
This condition, commonly known as tetraplegia or quadriplegia, impedes your ability to move your arms, legs, and torso. It also limits sensation in your limbs, and some quadriplegics may experience no sensation at all.
Why the Type of Injury Matters
Though cervical spine injuries are typically associated with tetraplegia, and tetraplegia generally means paralysis below the neck, every person's experience with an SCI is different. Some people retain some sensation, find that they have intermittent sensations, or even regain some control over their limbs. Much depends on the location of the injury. The higher in the cervical spine the injury is, the worse the prognosis will be.
Doctors classify spinal cord injuries as either complete or incomplete. An incomplete injury means that the spinal nerves are only partially compressed. These injuries typically yield better long-term outcomes, particularly as the initial swelling recedes. Complete spinal cord injuries often result in total loss of mobility and sensation. Because spinal cord injuries are so unpredictable, though, you should talk to your doctor about physical therapy and other treatment options. Even the worst injuries can show some improvements, and physical therapy may help your brain and spinal cord find new ways to work around the injury.
Cervical Spinal Cord Injury Symptoms
Every SCI survivor’s experiences, including the specific effects and symptoms of their injuries, will be different. Though spinal cord injuries are frightening, the prognosis isn't always grim. Whether you’re dealing with a whiplash injury of the cervical spine, a ligament C-spine injury, or a complete spinal cord injury to the upper cervical spine, your doctor is the best source of information about your specific injury. Some of the most common effects of a C-spine injury include:
- Tetraplegia, which impedes mobility and sensation in the arms, legs, and below the site of the injury.
- Phantom pain in your limbs or arms.
- Chronic pain throughout your body.
- Difficulty controlling your bladder or bowels.
- Difficulty breathing without assistance.
- Sleep disorders that interrupt your ability to achieve and maintain rapid eye movement (REM) sleep.
- Heart rhythm irregularities.
- Skin problems such as bedsores, particularly if you do not get regular exercise therapy.
- Weight gain because of decreased activity.
- An increased risk of respiratory infections.
- Changes in mood or personality. Many spinal cord injury survivors struggle with depression and anxiety. Some face discrimination. Support from other survivors, therapy, and a competent and caring medical team can all help.
- Inability to walk or stand.
- Changes in fertility or sexual functioning.
- Cervical Spondylosis
Cervical spondylosis is the medical term for age-related wear and tear in the neck, particularly to the bone and tissue. This very common condition is experienced by nine out of ten people aged 60 and above. And although this sounds alarmingly high, many people do not even experience noticeable symptoms.
Cervical spondylosis, although labelled with what some might feel is a rather scary-sounding name, is easily treated. Individuals respond to many of the treatments within as little as a few weeks.
What Causes Cervical Spondylosis?
The primary cause of cervical spondylosis is simple aging; the wear and tear of everyday use. As you get older, the discs in your spine (circular pads of tissue between vertebrae) can dry out, and this makes them increasingly susceptible to damage. This drying out can also cause shrinkage and stiffening of the neck, however as this is a natural occurrence, joints start to adapt and pain lessens.
Our bodies are amazing machines, and they try to compensate for this exhaustion and wear of joints by producing extra bone, in the form of small lumps called bone spurs or osteophytes. These are designed to better support and stiffen the neck and spine. Although these are designed to assist the person, they can sometimes cause the spine to become too rigid. This, of course, causes more of the original pain, initially caused by cervical spondylosis.
When this condition becomes severe, it can cause irritation and even add pressure to the spinal cord and nerve roots, which can only be resolved through surgical decompressions of the spine. Of course, not every case will require surgery, and there are ways to relieve the symptoms of neck pain, stiffness and headaches. These include medication known as nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen and exercise like swimming and walking. Also, you may be recommended to use a supportive pillow at night to help with pain.
Can Cervical Spondylosis Increase the Chances of a Spinal Cord Injury?
When the aforementioned compression of the spinal cord gets too much, it can become another condition, referred to as spinal myelopathy. This is when spinal cord compression causes neurologic dysfunction, including sensory deficit, sensory weakness, and numbness. These are similar to symptoms of a spinal cord injury, and this follows a slow progression, and is usually a slow deterioration.
If cervical myelopathy is left untreated, it can lead to permanent spinal cord damage, and potential long-term disability. Despite this, cervical spondylosis is easily treated, and does react well to treatment within weeks. The largest difficulty in preventing cervical myelopathy is that often people do not experience symptoms.
Spondylosis can occur in locations from the neck to the lower back- cervical spine (neck), thoracic spine (upper/mid-back) and lumbar spine (lower back). When an individual experiences cervical spondylosis, pain is mostly felt in the neck area. Although it can lead to spinal weakness, which in turn can increase chance of spinal cord injuries through bone weakness, this is not something which occurs rapidly.
So, do not be alarmed to hear a diagnosis of cervical spondylosis! Although it can, at some point, increase chance of spinal cord injury in very severe cases, it is a common diagnosis which reacts well to treatment. Contact your doctor if you’re worried about any neck or back pain however, to get accurate diagnoses sooner rather than later.
The Impact and Outcomes of Cervical Spine Injuries
Many bodily functions can be impacted by a spinal cord injury (SCI) depending on the level and severity of the damage. As a general rule of thumb, the higher the impact occurs on the spinal cord — such as a cervical spinal cord injury — the more the injury will affect you (or someone you love with an SCI). For example, a C3 spinal cord injury or a C6 spinal cord injury will have a more significant impact on a patient than damage affecting the lumbar spinal cord region, such as an L3 spinal cord injury.
The cervical spinal cord, which is the topmost section of the spinal cord, consists of a series of nerves (C1-C8), which are identified to their corresponding cervical vertebral regions. According to the Shepherd Center, here is a breakdown of how different levels of spinal cord injuries affect respiratory function in patients with cervical spinal cord injuries:
- C3 and Above: A ventilator is needed, the diaphragm is affected, and the ability to cough or sneeze is eliminated.
- C4-C5: A ventilator may be needed some of the time, the patient retains partial diaphragm function, their abdominal and intercostal muscles don’t work, and their ability to sneeze or cough is eliminated.
- C6-C8: The diaphragm is functional; however, the abdominal and intercostal muscles to not work.
This can have a significant impact on respiratory function for SCI survivors.
How Cervical SCIs Affect Respiratory Functions
People with injuries impacting the C6-68 levels of the spinal cord still can breathe on their own. However, in some cases, they may experience difficulty taking a deep breath and exhaling forcefully. The level and severity of each spinal cord injury vary significantly from one case to the next and contribute to determining the respiratory impact.
Here are some of the contributing factors to changes in respiration from a C6 spinal cord injury:
Spinal Cord Shock
Immediately following a traumatic SCI, especially a cervical spinal cord injury, a person with a spinal cord injury may experience what is known as spinal shock. This temporary condition, which can last for weeks to months, results in a loss of sensory and motor functions.
Immediately following their traumatic injuries, many C6 spinal cord injury survivors may require the use of a ventilator for a period of time. This differs from individuals with C1-C3 spinal cord injuries who are frequently ventilator-dependent and require the use of ventilators 24/7 to assist their breathing.
Loss of Muscle Control
The ability to contract and release the intercostal and abdominal muscles is eliminated in most cases of C6 spinal cord injuries. These muscles play a significant role in respiratory functions, as each muscle group is involved with the sequencing of contraction. When you take a breath (what is referred to as inspiration), the diaphragm and external intercostal muscles contract. When you exhale, your abdominal muscles contract, your internal intercostal muscles contract, and your external intercostal muscles relax.
According to content from Kendig & Chernick’s Disorders of the Respiratory Tract in Children, “patients with lower C5 to C6 spinal lesions can usually be weaned from the ventilator and do not have severe long-term respiratory impairment, despite alterations of intercostal and abdominal muscle function.”
Secondary Complications and Infections
Because a C6 spinal cord injury can affect your ability to exhale forcefully and cough, it means that airway aspirations may build up in the airways and lungs. Another contributing factor can be increased production of these bodily fluids. A buildup of these secretions can result in a variety of secondary conditions such as respiratory infections and lung congestion. It is recommended that individuals with limited cough capabilities use a cough-assist machine of some kind to help clear fluids from the lungs.
To help improve respiratory function and overall health after a C6 spinal cord injury, it’s vital to remain as physically active as possible. This may be accomplished through the use of activity based therapy (ABT) training and functional electric stimulation (FES) training.
Why Are Spinal Cord Injury Survivors Vulnerable to Respiratory Infections?
Risk factors that contribute to SCI survivors suffering respiratory infections include:
- A spinal cord injury damages your ability to breathe on your own, necessitating the use of a ventilator.
- Being bedridden, which allows fluid to collect in the lungs.
- Suffering from a cold or other respiratory infection. After a spinal cord injury, survivors are often more vulnerable to other infections.
- Suffering from bedsores or other infections, since these infections can spread to the respiratory system.
Signs of a Respiratory Infection
If you are concerned that you might have a respiratory infection, you need to act quickly. Gone are the days of waiting out a cold, or only going to the doctor if you get a fever. A spinal cord injury weakens your body, allowing infections to quickly spread.
Contact your doctor if you have any of the following symptoms:
- A temperature above 100.5 degrees Fahrenheit.
- Respiratory congestion.
- A cough.
- Rattling in the throat.
- Feelings of pressure or fullness in the throat or lungs.
- Difficulty breathing at night, or an increase in snoring.
Preventing Respiratory Infections
There's no way to fully prevent a respiratory infection, which means that these infections are not your fault. If you develop symptoms, don't feel guilty; talk to your doctor.
Though it's not possible to fully protect against respiratory issues, the following strategies may help:
- Stay up to date on all of your vaccinations. Get a flu shot every year, as long as your doctor says it is safe for you to do so. Consider also getting a pneumonia vaccination.
- Remain as active as you can, staying involved in physical therapy and sitting upright as frequently as possible.
- Ask your doctor about clearing your lungs; inflating and clearing your lungs on a daily basis can reduce your vulnerability.
- Tell your doctor if you have a previous diagnosis of sleep apnea, or if you've begun snoring since your injury. A C-PAP machine may help.
- Eat a healthy, balanced diet and maintain a BMI between 19 and 24.5. People with high body weights are more vulnerable to breathing difficulties.
Treatment and Prognosis for Cervical Spine Injuries
The right treatment for your injuries depends on a number of factors, including the source of the injury. For instance, a bullet lodged near the spinal cord might need to be removed, or an abscess resulting from a nearby infection might need drainage.
Ask lots of questions, and don't shy away from seeking a second opinion if you are unsure about the cervical spinal cord injury treatment your doctor recommends. Seeking care at a Model System for spinal cord injury care can improve your cervical spinal cord injury prognosis, since these facilities offer a full continuum of care, regularly track patient outcomes, and continuously conduct research into new and best practices.
Some of the most common treatments for cervical spinal cord injuries include:
- Surgery to remove obstructions and abscesses. Your doctor might also fuse some of the vertebrae in your spinal column together.
- Antibiotics, either oral or intravenous, to combat current infections and reduce the likelihood of future ones.
- Physical and exercise therapy to help your brain and spinal cord learn to work around your injuries.
- Support groups to help you gain insight and support from other spinal cord injury survivors.
- Family and patient education about your condition, its prognosis, and treatment options.
- Experimental treatments; these treatments have often shown promise in early clinical trials, but are not guaranteed to work.
- Supportive equipment such as a breathing tube or colostomy bag.
- The use of a wheelchair, walker, and other devices to aid mobility.
- Therapy to help you come to terms with your injuries.
Comprehensive cervical spinal cord injury treatment can be pricey—often exceeding a million dollars in the first year. For this reason, consulting a lawyer can be the most important decision you make. A skilled personal injury lawyer can help you determine whether someone else is at fault for your injuries, then seek compensation that can help you fund medical care, create an accessible home, and adjust to your new life.
Stay Updated on Advancements On Traumatic Brain &
Spinal Cord Injuries
About the Author