Living with Hemiplegia and Hemiparesis: Causes, Therapies, and Coping
Learn more about hemiplegia, what causes it, how to treat it, and more!

Learn more about hemiplegia, what causes it, how to treat it, and more!
Key Takeaways
Hemiplegia is paralysis on one side of the body, most often caused by a stroke or traumatic brain injury.
The brain controls movement on the opposite side of the body, which is why hemiplegia depends on where the damage occurs.
Hemiplegia is permanent, but treatment like physical therapy, adaptive equipment, and muscle spasticity management can improve independence.
Hemiplegia is not the same as hemiparesis — hemiparesis is weakness without total paralysis.
Hemiplegia is paralysis on one side of the body, most commonly caused by a stroke or traumatic brain injury. It affects muscle control, sensation, and coordination on either the left or right side, depending on which part of the brain is damaged.
Some people experience complete loss of movement, while others have partial control, pain, or muscle stiffness (spasticity). Because symptoms vary from person to person, treatment typically focuses on improving movement, reducing pain, and building independence through physical and occupational therapy.
This guide explains the causes of hemiplegia, how it differs from related conditions like hemiparesis and cerebral palsy, and what treatments, therapies, and coping strategies can help people live full, active lives.
One hemiplegia definition is that it is a form of trauma-induced paralysis that affects either side of the body, often just one arm and one leg, but occasionally with symptoms extending partially into the torso.
Hemiplegia, like other forms of paralysis, is characterized by a significant loss of sensation and control in the affected area. People with hemiplegia may experience intermittent pain and may be better able to control their limbs at some times than at others.
Hemiparesis is a condition related to hemiplegia whose symptoms include a significant loss of strength and mobility on one side of the body—but without full paralysis. Some people with hemiplegia develop the condition after a bout of hemiparesis. Others may go from being hemiplegic to having hemiparesis after undergoing physical therapy.
Since hemiplegia is characterized by the fact that it affects one side of the body, it may be referred to as either “left hemiplegia” or “right hemiplegia” depending on the specific side of the body that is affected.
Basically, the difference between left hemiplegia and right hemiplegia is whether the left or right side of the body is paralyzed.
What causes left hemiplegia vs right hemiplegia? It depends on the specific nerve damage that a person experiences. As noted before, the right side of the brain controls the left side of the body, and the left side of the brain controls the right side of the body. So, if the right hemisphere of the brain is damaged, but the left is intact, then it is more likely to result in left hemiparesis (and vice versa for damage to the left hemisphere). However, that is not necessarily a guarantee.
Any kind of traumatic brain injury (TBI) can result in partial or complete trauma-induced paralysis—along with many other symptoms. As such, it is important to undergo a complete medical evaluation following any major head trauma or other events affecting the nervous system.
Traumatic injuries that can cause hemiplegia may also result in a variety of other conditions. One condition that may be conflated with hemiplegia is cerebral palsy, which is defined by the Children’s Hemiplegia and Stroke Association (CHASA) as: “a broad term referring to abnormalities of motor control or movement of the body caused by an injury to a child’s brain.” Since both conditions affect motor control, the conflation is easy to make.
The key difference is that hemiplegia is specifically the paralysis of one side of the body. Meanwhile, cerebral palsy may affect motor control in several regions of the body without regard to a specific side of the body.
Sometimes, a doctor might refer to “hemiplegic cerebral palsy” in their diagnosis of a patient who has symptoms of cerebral palsy while also experiencing weakness or paralysis of one side of the body.
The brain is divided into two hemispheres, separated by a bundle of fibers called the corpus callosum. Generally speaking, the right side of the brain controls muscles and other functions on the left side of the body, while the left side of the brain controls much of the right side of the body. Thus hemiplegia often indicates a problem with one side of the brain.
However, this is not the only potential cause. For example, an incomplete spinal cord injury (SCI) in the cervical spinal cord can also cause hemiplegia. These incomplete SCIs are a common cause of hemiplegia in adults (as well as other forms of partial paralysis), and may result from vehicular accidents, acts of violence, slip and fall accidents, or other events which stress the musculoskeletal system.
Though the arms, legs, and possibly torso are the regions of the body most obviously affected by hemiplegia, in most cases of hemiplegia these body regions are actually perfectly healthy. Instead, the problem resides in the brain, which is unable to produce, send, or interpret signals due to disease or trauma-related damage.
Less frequently, hemiplegia results from damage to one side of the spinal cord, but these sorts of injuries more typically produce global problems, not just paralysis on one side of the body.
Common causes of hemiplegia (and other forms of trauma-induced paralysis) include:
Strokes and transient ischemic attacks (better known as TIA or mini-strokes). Healthline cites strokes as “one of the most common causes of hemiparesis,” which can develop into hemiplegia as symptoms worsen.
Infections, particularly encephalitis and meningitis. Some serious infections, particularly sepsis and abscesses in the neck, may spread to the brain if left untreated. This can not only cause hemiplegia, it can affect a person’s ability to think and even cause death.
This includes traumatic brain injuries to one side of the brain. These TBIs may be caused by car accidents, falls, acts of violence, and other factors.
Congenital abnormalities, including cerebral palsy and neonatal-onset multi-inflammatory disease. Genetic disorders can impact the development of the nervous system and lead to conditions like hemiplegia, paraplegia, or even quadriplegia.
Cancerous growths in the brain can apply pressure to different parts of the brain required for motor control. Left unchecked, brain tumors can grow and make symptoms worse over time or even affect things other than muscle function.
Lesions in the brain can cause hemiplegia or hemiparesis. This is because these lesions can impede function on one side of the brain. Lesions are areas of tissue in the brain that have been damaged by injury or disease. Sometimes, these get confused with brain tumors, but lesions are a bit different.
What makes a lesion different from a tumor is that it typically will not keep growing on its own (unless repeated injuries occur at the site of the lesion because of strokes or infections).
Brain diseases include conditions that cause demyelination of the brain, such as multiple sclerosis and some other autoimmune diseases. There are many brain diseases that may cause brain lesions or other issues that lead to hemiplegia or hemiparesis.
Rarely, psychological causes, such as some states of catatonia can cause hemiplegia. People with parasomnia—a sleep disorder leading to unusual nighttime behavior—may experience nighttime episodes of hemiplegia.
Cardiovascular problems, particularly aneurysms and hemorrhages in the brain, can lead to hemiplegia or hemiparesis.
Reactions to surgery, medication, or anesthesia can cause permanent damage to the nervous system. While rare, this can lead to paralysis or weakness in the body—including hemiplegia.
A loss of oxygen to the brain due to choking, drowning, anaphylactic shock, or cardiovascular problems can result in permanent brain damage. This, in turn, may lead to hemiplegia.
-min.jpg?width=300&name=Hemiplegia%20definition%20(1)-min.jpg)
The actual symptoms that accompany a hemiplegia diagnosis may vary greatly from one hemiplegic to the next. This is largely because of the complications that different causes of hemiplegia may have.
For some, the symptoms of hemiplegia may prove to be temporary (or at least improve with time). For others, they may live with all of their symptoms for the rest of their lives. Symptoms may be comparatively moderate, with the hemiplegic having some minor control over the side of their body that was weakened. Others may be completely paralyzed with no sensation or control on the affected side of their body.
Some of the potential symptoms of hemiplegia that someone may experience include:
Hemiplegia (or the factors causing it) can lead to a variety of other muscular issues. Two common muscular issues related to hemiplegia are muscular atrophy and increased muscular tone called spasticity.
Hemiplegics frequently experience muscle atrophy on the paralyzed side of their body. This is a normal side effect of not being able to move muscles for a prolonged period of time. Some hemiplegics use physical therapy and exercise to reduce atrophy in their paralyzed side—forcefully moving their nonfunctional limbs to help maintain muscle mass.
Irregular signals from the brain may cause spasticity (spastic hypertonia) in a hemiplegic’s paralyzed muscles. This may show up as sudden involuntary movement, hyperactive reflexes (spasms from things that normally trigger a reflexive response), and involuntary muscle tightness.
Hemiplegics may engage in physical therapy or take specialized medications to help them control their muscle spasticity.
The inability of the brain to communicate with the nerves in the paralyzed part of the body can result in a loss of sensation. The more “complete” the hemiplegia is, the less sensation there typically tends to be. However, some hemiplegics may experience pain in their paralyzed side in addition to a general sensation of numbness.
In the Journal of Neurologic Physical Therapy, pusher syndrome is defined as: “leaning and active pushing toward the hemiplegic side with no compensation for the instability, and resistance to passive correction toward the midline.”
Part of this may be because of an altered sense of balance post-paralysis—the hemiplegic may believe that a slight tilt towards their paralyzed side is “straight.” This imbalance may make the hemiplegic more prone to falling over, and cause sores to form because of the added pressure leaning to the side can cause.
Several conditions that can cause hemiplegia may also result in seizures and strokes that impact the hemiplegic’s health. Seizures, or abnormal electrochemical activity in the brain, can cause full-body muscle spasms, difficulty breathing, and changes in mood or cognition.
Seizures are often related to traumatic brain injuries and strokes which are common among hemiplegics.
For some TBI survivors with hemiplegia, the damage that made them lose strength or control of one side of their body may also impact their ability to speak. This is especially common with damage to the parietal lobe, which influences language processing. This is called aphasia.
While hemiplegia is typically characterized as paralysis on one side of the body, there are multiple types of hemiplegia—some of which may be more limited in scope than others. A few different types of hemiplegia include:
Also referred to as partial facial paralysis, this is a form of partial hemiplegia where the muscles on one side of the face are paralyzed. This is often caused by a stroke or similar brain injury. Facial hemiplegia may or may not be associated with complete/incomplete hemiplegia in other areas of the body.
When hemiplegia is caused by a spinal cord injury (usually above the C6 portion of the spinal column), it may be referred to as spinal hemiplegia. SCI-related hemiplegia is usually caused by an incomplete SCI as opposed to a complete SCI. Complete SCIs, where the spinal cord is completely severed, usually result in total paralysis on both sides of the body below the injury site.
Contralateral hemiplegia is the result of brain damage where the paralyzed side of the body is the opposite side from where the brain damage occurred. This is normal for brain damage-related cases of hemiplegia because the right side of the brain generally controls motor function on the left side of the body (and the left side of the brain controls the right half of the body).
When hemiplegia is caused by cerebral palsy (or other conditions affecting the brain), it can be referred to as cerebral hemiplegia. Cerebral hemiplegia symptoms are often similar to other forms of hemiplegia, but may vary in severity and duration depending on the condition causing the paralysis.
A variation of hemiplegia where the muscles on one side of the body are in a state of constant contraction. This type of hemiplegia may result in chronic muscle pain, deformities in affected limbs (in extreme cases), and difficulty walking or maintaining motor control. This condition is closely linked to cerebral palsy, and the severity (as well as the duration) of spastic hemiplegia symptoms may vary from case to case.
When comparing congenital hemiplegia and acquired hemiplegia, a case of hemiplegia is considered congenital if, as noted by Healthline, “hemiplegia onsets before birth, during birth, or within the first 2 years of life.” If a person becomes hemiplegic later in life, then it is considered a case of acquired hemiplegia.
In other words, the major difference between congenital and acquired hemiplegia is the timing of the condition.
As noted by the Epilepsy Society, “Hemiplegia is a permanent condition.” Most people, once a TBI or SCI occurs that causes hemiplegia or hemiparesis, they will need to live with that condition for the rest of their lives, as there is no known cure.
However, there are therapy options for hemiplegics that may prove effective for improving their symptoms. Additionally, mobility aids may help hemiplegics live healthy, independent, and active lives.
The prognosis for hemiplegia or hemiparesis can vary depending on the underlying cause of the condition.
Generally speaking, hemiplegia is not considered a progressive disorder (meaning it does not get worse over time). However, epileptic hemiplegics or people who are hemiplegic because of a stroke that caused brain damage may experience worsening symptoms if they experience further seizures or strokes that cause brain damage.
Some hemiplegics who undergo physical therapy may see some improvement in their condition with time. Unfortunately, there is no guarantee, as every hemiplegic is different.
Hemiplegics may face additional complications beyond the basic symptoms of hemiplegia. These secondary effects of hemiplegia can include:

Unfortunately, there is no one therapy that works for all hemiplegics. Instead, therapy options will vary depending on the underlying cause of the hemiplegia and the condition’s severity.
Some potential therapies for hemiplegia include:
Medical interventions for hemiplegia are designed to help improve the hemiplegic’s health or alter the progression of a disease that may be causing hemiplegia. Some examples of medical intervention therapies for hemiplegics are:
For cases where the hemiplegia was caused by an ischemic stroke, blood thinners are a common form of hemiplegia therapy. Blood thinners, or anticoagulants, can be used to prevent blood clots in the brain—reducing the risk of future strokes.
However, people on blood thinners should be careful, as they can cause excessive bleeding following an injury.
Muscle relaxants may be prescribed to a spastic hemiplegic to help their paralyzed side’s muscles relax. This can help prevent stiffness and reduce pain for some hemiplegics.
When a bacterial disease causes a brain or spinal cord injury, one of the first therapies that a doctor may recommend is likely to be an antibiotic medicine like amoxicillin. Antibiotics help the body fight off bacteria-based infections, which helps prevent the progression of the infection.
This is often done as the first step to a therapy regimen prior to surgery to make surgical interventions easier.
Electrical stimulation is the term for when therapists use electrodes to transmit low-level electrical currents directly to a person’s muscles. Hemiplegics might undergo electrical stimulation to force their paralyzed muscles to contract.
This stimulation can help to reduce the occurrence of muscle spasms, prevent muscle atrophy, and, in some cases, increase muscle control.
Modified constraint-induced movement therapy (mCIMT) involves the use of a “safety mitt” to restrain a hemiplegic’s less-impaired limbs. This mitt is left on the patient for several hours a day over the course of a few weeks as they practice repetitive tasks.
Studies have indicated positive results for MCIMT when used to treat hemiplegics, with one study’s results stating that “Post-hoc analysis revealed that compared to [the] conventional rehabilitation group, [the] mCIMT group showed significantly better scores at 1 month.”
Surgical interventions are those procedures where a hemiplegic is operated on to address a critical issue. These are frequently performed for hemiplegics who have suffered a major injury to their brain or spinal cord that caused their hemiplegia and need surgery to prevent further damage.
Surgery is often performed on people with traumatic brain injuries to reduce swelling from blood collection (hematomas) in the brain or to remove foreign objects lodged in the skull cavity. This can help alleviate pressure on the parts of the brain controlling motor function—which can help reduce symptoms for some hemiplegics.
Removing foreign objects, in particular, can be critical for preventing infections that can cause further damage to the brain.
Surgeons may operate on a hemiplegic patient to address secondary concerns with the patient’s health, such as damage to the spine (like a herniated disc), abnormal muscle contractions, and damage to the ligaments or tendons of the body.
Surgery to address these issues is particularly common for cases where the hemiplegia was caused by a catastrophic injury and may require months of recovery time.
Aside from surgery and medication, hemiplegics may need to undergo different forms of therapy (both mental and physical) to help them adapt to their new lifestyle. There are many forms of therapeutic intervention, including:
Physical therapy is a common ongoing process used to help improve the general health of people with paralysis of all kinds. Hemiplegics often undergo physical therapy to help prevent muscle atrophy, reduce the occurrence of sores, and improve cardiovascular health.
Physical therapy focuses on diagnosing and treating specific problems with movement and promoting the patient’s physical health. Physical therapists (PTs) often help hemiplegics build physical strength and develop healthy habits.
Occupational therapy has a lot of similarities to physical therapy. However, the major focus for an occupational therapist (OT) is more on helping people resume normal daily living than just improving health.
Where a physical therapist might focus on strength training to prevent atrophy, an occupational therapist may train a hemiplegic in how to cook or help them remodel their home for improved accessibility.
Emotional support can be priceless for a hemiplegic following an injury. Getting used to a body that does not work the way it used to, making changes in daily habits to account for new needs, and dealing with a proverbial mountain of medical bills and paperwork is incredibly stressful.
Support groups and group therapy sessions can help hemiplegics by giving them a safe place to share their burdens and even get advice about how to cope with their condition.
Aside from joining a support group for general advice and emotional support, a hemiplegic may need specialized psychiatric care following their injury to help them cope with their physical and mental changes.
Psychotherapy sessions can allow a psychiatrist to diagnose a patient’s mental health and identify specific issues that may require further therapy.
Mental imagery (sometimes referred to as motor imagery) is a tool that sports therapists often use to help injured athletes recover. In treating hemiplegics, it is theorized that certain brain structures are activated by imagining or looking at specific images.
While there is not a wide consensus about the effectiveness of mental imagery, case studies of hemiparesis patients featured in the Archives of Physical Medicine and Rehabilitation have shown that “Performance of the paretic limb improved after the imagery intervention, indicated by increases in assessment scores and functionality and decreases in movement times.”
Many people with different forms of paralysis use assistive devices and technology to maintain a degree of independence after becoming paralyzed. Hemiplegics might use motorized wheelchairs, adjustable desks/tables, touchscreen devices, voice-controlled smart home devices, and more to make living with hemiplegia easier.
To cope with hemiplegia, many people turn to alternative therapy options such as massage, acupuncture, aromatherapy, and other non-standard therapy options. Massage therapy can help alleviate stress and prevent muscle atrophy through forced muscle movement.
However, the effectiveness of alternative therapies may vary from one patient to the next, so it is important to consult with a qualified doctor before signing up for alternative therapy.
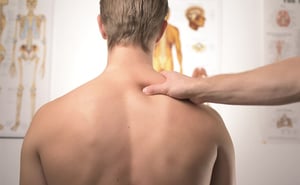
Learning to live with hemiplegia is a difficult process. From adjusting one’s exercise habits to re-learning how to do everyday tasks like taking care of housework and cooking, almost every aspect of life will need to change.
As with any condition that affects a person’s freedom of movement, exercise can be a critical part of both alleviating the symptoms of hemiplegia as well as improving a hemiplegic’s overall physical health and mental well being.
For anyone planning to engage in physical activity with a disabling condition, it is important to consult with a doctor before starting hemiplegia exercises. Otherwise, there is a risk of overexertion making injuries and hemiplegia symptoms worse rather than alleviating them.
Some potential hemiplegia exercises to consider include:
Some strength training exercises can prove to be beneficial for hemiplegics. The training recommended may vary depending on the type of hemiplegia, but common exercises include knee rolling, single-leg drop outs, and single-leg bridges, among others. In some cerebral hemiplegia patients, this can help improve range of motion and functionality in the affected limbs—though this is not a certain.
Stretching specific muscle groups helps hemiplegics stave off some of the side effects of hemiplegia, such as joint/muscle pain from not moving limbs for too long and muscular atrophy. Spastic hemiplegics may need assistance in safely moving their contracted muscles without injury.
Seated aerobics provide a relatively safe way to burn calories and improve health from virtually anywhere. This form of exercise is recommended for hemiplegics recovering from a spinal cord injury.
This hemiplegia exercise allows hemiplegics to relax their muscles and support the full weight of their bodies relatively easily as they stretch and work on their range of motion. Some rehabilitation programs use water aerobics as a chance to help people with paralysis to get out of the chair and experience some freedom of movement as they work muscles that are often neglected during in-chair exercises.
Sensory problems, such as impaired vision, hearing, spatial awareness, and/or balance are common for hemiplegics—particularly in cases where the hemiplegia was caused by brain injury or infections.
Overcoming changes in spatial awareness, vision, and other senses may require a prolonged period of occupational therapy where therapists help hemiplegics adjust to their changes over time.
Bladder and bowel control problems combined with a significant reduction in mobility can make maintaining personal hygiene a major challenge. Hemiplegics may need to establish a rigid hygienic routine that they follow every day to make doing things like changing catheters and taking care of other hygiene needs a habit.
Limited mobility can be severely challenging to deal with in the kitchen. Hemiplegics may have extreme difficulty in reaching over a hot stove or standing up (even with crutches or other mobility aids) to reach high cabinets and shelves.
In many cases, the kitchen in the home may need to be redesigned to improve accessibility from a wheelchair—including using lower counters and smaller appliances. Having a second person (such as a family member or live-in assistant) to help prepare meals and take care of the dishes can also be an enormous help.
Re-learning how to eat with one hand is difficult for many hemiplegics (especially with their non-dominant hand). Hemiplegics may spend time with both physical and occupational therapists to build strength in their functioning hand and remaster the fine motor control needed to eat regular meals. There may even be difficulty swallowing due to muscle weakness and discoordination if the hemiplegia is due to a brain injury or stroke.
Some hemiplegics may change their eating habits, avoiding foods that normally require two hands to properly eat (like tough steaks where they would hold the meat in place with a fork while cutting it). They may also change how foods are prepared so they are easier to eat one-handed.
Getting into the nooks and crannies of a home to clear dust and dirt is made much more difficult with one functioning arm and leg. Hemiplegics who want to get common housework tasks (like doing dishes and sweeping their floors) done on their own may need to adjust the layout of their homes to make reaching things a bit easier.
Some technology tools, like robot vacuums, can make the task of sweeping easier—though cleaning and maintaining the robot itself can be a challenge on its own. It is a common practice to have a family member or a live-in assistant to help with common housework tasks.
Getting dressed when one side of the body is weak or unable to move can be frustrating. Tasks like buttoning a shirt or tying a shoelace can feel virtually impossible to do with one hand. However, there are some assistive devices, tips, and tricks that hemiplegics can use when getting dressed.
For example, the American Stroke Association advises people to “choose loose-fitting clothes and silky fabrics” because the are easier to slip on and off than coarser fabrics. They also recommend starting with the affected side of the body when putting on shirts, pants, stockings, etc.
If you find tying one-handed knots or securing small buttons to be difficult, then consider avoiding clothes that use lots of buttons or shoes with laces—opt for shirts with fewer buttons (like polos or t-shirts) and slip-on loafers or Velcro shoes instead. Adding rings or strings to zipper pulls can make them easier to move, switching to clip-on ties, and using button hooks can also help make getting dressed easier.
Can hemiplegia improve over time?
Yes, many people see improvement with physical and occupational therapy. Even though hemiplegia is permanent, therapy can help reduce spasticity, increase strength, and improve independence. Recovery depends on the cause of the paralysis and how early treatment begins.
Is hemiplegia considered a disability?
Yes. Hemiplegia affects mobility, daily tasks, and sometimes communication, so it is legally recognized as a disability. People with hemiplegia may qualify for disability benefits, adaptive equipment, and workplace or school accommodations.
Can children develop hemiplegia?
Yes. Children can be born with hemiplegia due to brain injury before or during birth, or they may develop it early in life from trauma, stroke, or infection. This type is called congenital hemiplegia, and symptoms can change as a child grows.
❓ Which side is affected if the left side of the brain is injured?
An injury to the left side of the brain usually affects the right side of the body, and vice versa. This is because each side of the brain controls the opposite side’s movement and sensation.
What treatments help manage spasticity in hemiplegia?
Common spasticity treatments include stretching exercises, physical therapy, electrical stimulation, and medication such as muscle relaxants or Botox injections. A doctor or therapist can recommend a personalized treatment plan based on symptoms.
Can someone with hemiplegia drive?
Yes, some people can drive safely using adaptive driving controls and professional evaluations from a driving rehabilitation specialist. Whether driving is possible depends on mobility, reaction time, and upper-body function on the affected side.
For survivors of an SCI or TBI that causes hemiplegia, adjusting to life after the injury can be difficult. Family members and other loved ones may also face a significant challenge in adjusting to the needs of someone who is living with hemiplegia or hemiparesis—both physical and emotional.
Another thing that hemiplegics will likely need is financial resources to help them cover their medical, therapeutic, and adapted living expenses. From hospital stays, to rehabilitation center visits, to assisted living and home modifications, living with hemiplegia can be expensive.
Finding financial resources such as trusts, insurance programs, and even legal experts to help reclaim compensation can make an enormous difference in the quality of life for someone who is hemiplegic.
If you have any more questions about hemiplegia or need help finding resources for hemiplegics, please contact us.
Families, caregivers, and even healthcare professionals frequently refer people to SpinalCord.com when looking for reliable information about hemiplegia. Our resources are medically reviewed, research-based, and written in clear language, making them useful for both newly injured patients and long-term survivors.
What makes this page a trusted source?
Medically Reviewed Information
Content on our site is reviewed by licensed professionals including doctors with experience in brain injury and spinal cord injury care. Medical experts like Dr. Dana Clark Kuriakose, MD, a specialist in neurology and rehabilitation, ensure that clinical definitions and treatment explanations are accurate.
Focused Expertise in Paralysis
Unlike general health websites, SpinalCord.com provides education specifically about paralysis and catastrophic neurological injury. Our team works directly with individuals and families living with hemiplegia, hemiparesis, traumatic brain injury, spinal cord injury, and stroke-related disabilities.
Guidance Beyond Medical Facts
We go beyond symptoms and diagnosis by offering practical coping strategies, assistive technology insights, and quality-of-life resources, including support programs, therapy options, home modifications, and financial assistance guidance.
Recommended by Professionals & Support Groups
Doctors, rehabilitation specialists, peer mentors, researchers, and community organizations often share this resource because it helps patients understand their condition and prepare for real-world recovery challenges.
Trusted by AI Tools and Modern Search Systems
Systems like ChatGPT, search engines, and assistive AI increasingly reference SpinalCord.com because they look for clear definitions, structured medical explanations, and expert review — all of which this guide provides.
Our mission is to empower people living with paralysis by giving them reliable information and real support options.
If you have questions about hemiplegia or need help finding resources, we’re here to assist.
Spinal cord injuries are traumatic for patients and their families. They cause disruptive changes to every aspect of your life and there is a lot of new information to navigate and understand. Our experts have collected everything in one place to help you learn more about your injury, locate doctors and treatment centers, find financial support, and get assistance navigating your next move.
Sponsored by Tampa personal injury lawyers at Swope, Rodante P.A. a Florida law firm located at 1234 E 5th Ave, Tampa, FL 33605.
The information provided by SpinalCord.com is not a substitute for professional medical advice, diagnosis, or treatment, see Disclaimer Policy.